Evaluation of Exacerbated Lactate as a Biomarker for Sudden Unexpected Death in Epilepsy (SUDEP) Using Two Mouse Models
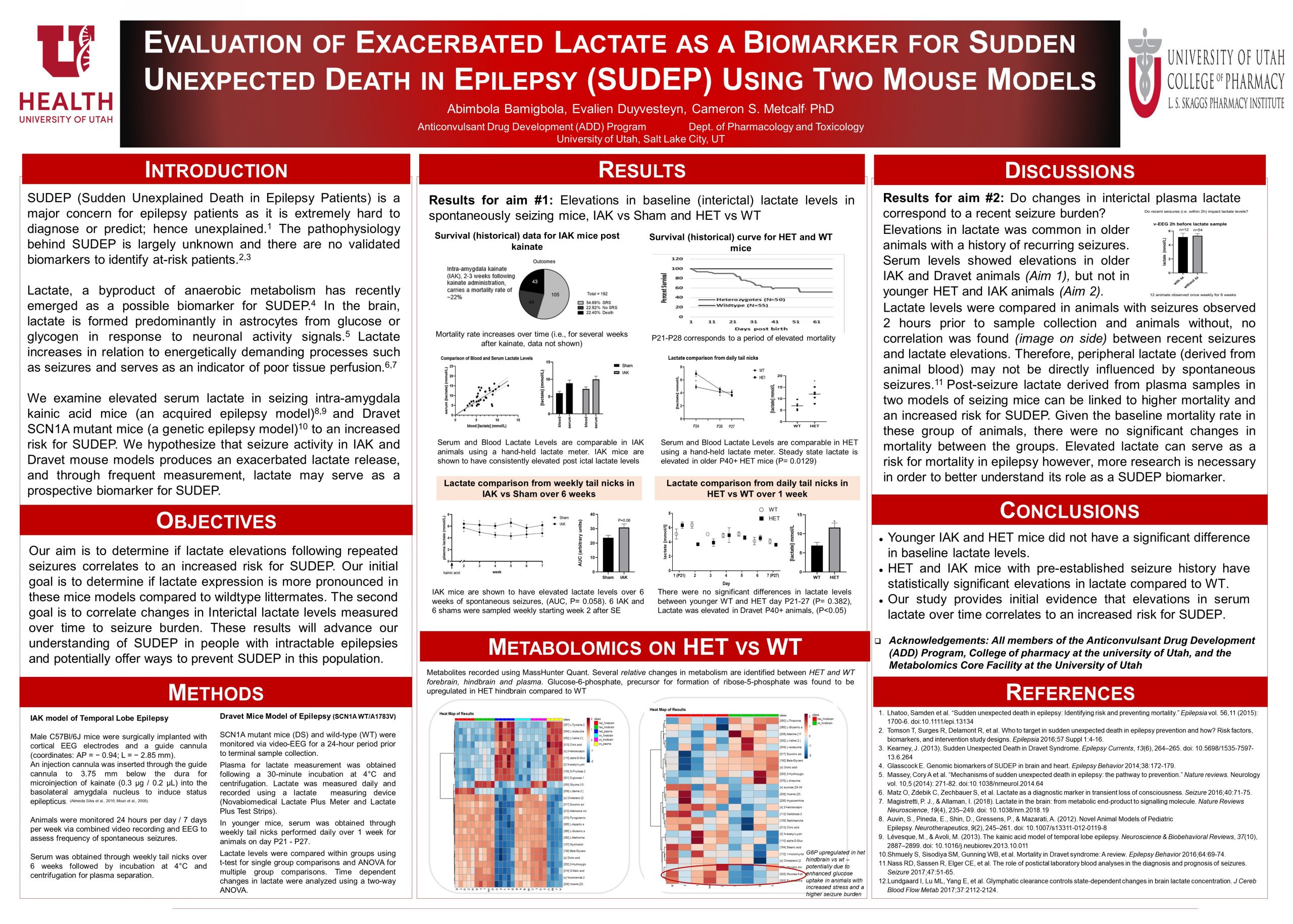
Purpose: SUDEP (Sudden Unexplained Death in Epilepsy Patients) is a major concern for epileptic patients with refractory seizures. The pathophysiology behind SUDEP is largely unknown and there are no validated biomarkers to identify at-risk patients. Lactate, a byproduct of anaerobic metabolism has recently emerged as a possible biomarker for SUDEP. In the brain, lactate is formed predominantly in astrocytes from glucose or glycogen in response to neuronal activity signals. It increases in relation to energetically demanding processes such as seizures and serves as an indicator of poor tissue perfusion. Lactate expression following seizures may therefore be indicative of pathological processes that contribute to recurring seizure activity and SUDEP risk. This study explores serum lactate as a potential biomarker for SUDEP. We examine the association of lactate in seizing intra-amygdala kainic acid mice (an acquired epilepsy model) and Dravet SCN1A mutant mice (a genetic epilepsy model) to an increased risk for SUDEP. We hypothesize that lactate levels following repeated seizures will be elevated, thus providing a potential biomarker for SUDEP.
Methods: The objective of the study is to determine if lactate can serve as a measurable biomarker predictive of SUDEP. Weekly blood samples were collected from IAK model mice (kainate induced C57BL/6) and Dravet model mice (SCN1AWT/A1783V) for 6 weeks. Animals were monitored 24 hours daily via video-electroencephalogram to assess frequency and length of spontaneous seizures. Serum was obtained through weekly tail nicks performed for 4 weeks on each animal or through terminal collection (following a 30-minute incubation at 4°C and centrifugation). Lactate was measured using a hand-held measuring device (Novabiomedical Lactate Plus Meter and Lactate Plus Test Strips). Seizure burden (recent) was compared to serum lactate, and trends were used to quantify lactate as a biomarker.
Results: Lactate was elevated at baseline in the two mouse models of epilepsy. Serum levels showed elevations in older animals with a history of recurring seizures (Aim 1, IAK AUC, P =0.58, HET AUC, P =0.013). In animals monitored daily for 6 weeks (Aim 2), no significant changes in lactate was observed. In animals, IAK and HET without an established seizure history, monitored daily for 6 weeks post kainate and HET monitored daily for 7 days, P21-27, lactate did not directly correlate to recent seizure burden. Given the baseline mortality rate in these group of animals, there were no significant changes in mortality between the groups.
Conclusion: The study provides initial evidence that an increase in serum lactate correlates animals with pre-established seizure history to an increased risk for SUDEP. Elevated lactate can serve as a risk indicator for mortality in epilepsy however more research is warranted on these mice models to make conclusion on its use as a SUDEP biomarker. Lactate should be closely monitored in patients with refractory seizures and the measurements should be used as a guide for clinical decision making.
Published in College of Pharmacy, Virtual Poster Session Spring 2020
This is an amazing finding. Thanks.
Thank you.
Abi, this is a very nice poster. Thank you. I am intrigued by how one can then go about really testing a causal link between the serum lactate and SUDEP. Do you think that’s necessary, or is it enough, when developing a biomarker, to simply have the association?
Hello Dr. Keefe, I think the link is lactate levels coupled with spontaneous seizures. Lactate is a commonly used biomarker that indicates high risk of mortality in other disease states. For example, in traumatic brain injury, elevations in extracellular lactate is associated with an unfavorable clinical outcome. This is why we thought to evaluate this association in SUDEP
Very interesting! I was wondering if applied to larger animals or clinical setting, if lactate would serve as enough of a surrogate to associate with increased risk of SUDEP? I tend to think there are many other reasons for lactate elevations in these clinical scenarios, that alone cannot be fully reliable, however this is a very interesting laboratory finding. What was the absolute number of seizures in the group with higher lactate vs the other group? I would be curious if it there is more of an association with the absolute number of seizures and EEG changes, than lactate. Thank you!
Hello Kimmy, I definitely think so, I would start with a larger group of animals. The absolute number of seizures in the higher lactate group was about 8 vs. 0-2 per day. We did this in a cohort of 6 animals per sample size for 6 weeks and not all the animals that received kainate grew to develop seizures. Usually when animals were having a lot of seizures(>17/day) we notice they would stop eating and die, so it would be really interesting to see what other causes account for elevated lactate in a clinical setting.
Hi Abi and nice work. I have a few questions. Did any of the IAK animals die during the experiment? Also, did you also do video EEG of the Dravet mice? Finally, what do you conclude about the metabolomics data? Thanks!